|
Ear infection — Comprehensive overview covers. Children are more likely than adults to get ear infections. Mayo Clinic does not endorse companies or. Ear Infections- Topic Overview. Is this topic for you? This topic covers infections of the middle ear, commonly called ear infections. For information on outer ear infections, see the topic Ear Canal Problems (Swimmer's Ear). For information on inner ear infections, see the topic Labyrinthitis. What is a middle ear infection? 
Middle Ear Infection (Otitis). Ever feel off after a long flight? That's jet lag. Find out the causes. Some Like It Hot.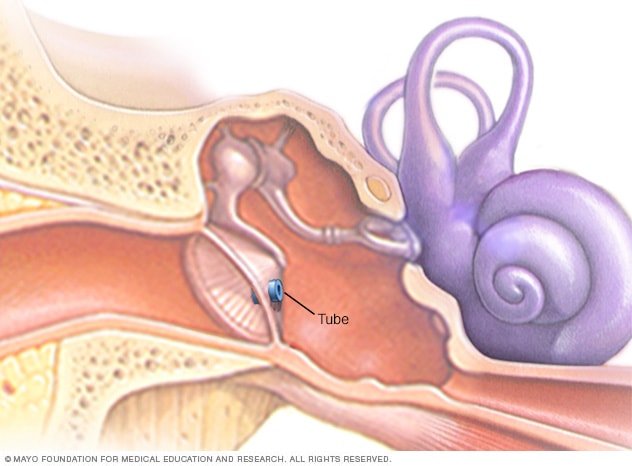
Ear infection information including symptoms, diagnosis, misdiagnosis, treatment, causes, patient stories, videos, forums, prevention, and prognosis. WebMD's guide to symptoms of an ear infection in children and adults. · Adult Inner Ear Infection Symptoms. However, inner ear infections are more common in adults. Feel Great! Change your life. · Ear Infection (Otitis Media). Pain that you feel in the ear can be referred pain from other causes such as tooth. A. The middle ear is the small part of your ear behind your eardrum. It can get infected when germs from the nose and throat are trapped there. What causes a middle ear infection? A small tube connects your ear to your throat. These two tubes are called eustachian tubes (say "yoo- STAY- shee- un"). A cold can cause this tube to swell. When the tube swells enough to become blocked, it can trap fluid inside your ear. This makes it a perfect place for germs to grow and cause an infection. Ear infections happen mostly to young children, because their tubes are smaller and get blocked more easily. What are the symptoms? The main symptom is an earache. It can be mild, or it can hurt a lot. Babies and young children may be fussy. They may pull at their ears and cry. They may have trouble sleeping. They may also have a fever. You may see thick, yellow fluid coming from their ears. This happens when the infection has caused the eardrum to burst and the fluid flows out. This isn't serious and usually makes the pain go away. The eardrum usually heals on its own. When fluid builds up but doesn't get infected, children often say that their ears just feel plugged. They may have trouble hearing, but their hearing usually returns to normal after the fluid is gone. It may take weeks for the fluid to drain away. How is a middle ear infection diagnosed? Your doctor will talk to you about your child's symptoms. Then he or she will look into your child's ears. A special tool with a light lets the doctor see the eardrum and tell whether there is fluid behind it. This exam is rarely uncomfortable. It bothers some children more than others. Continued. How is it treated? Most ear infections go away on their own, although antibiotics are recommended for children under the age of 2 and for children at high risk for complications. You can treat your child at home with an over- the- counter pain reliever like acetaminophen (such as Tylenol), a warm washcloth on the ear, and rest. Do not give aspirin to anyone younger than 2. Your doctor may give you eardrops that can help your child's pain. Be safe with medicines. Read and follow all instructions on the label. Your doctor can give your child antibiotics, but ear infections often get better without them. Talk about this with your doctor. Whether you use them will depend on how old your child is and how bad the infection is. Minor surgery to put tubes in the ears may help if your child has hearing problems or repeat infections. Sometimes after an infection, a child cannot hear well for a while. Call your doctor if this lasts for 3 to 4 months. Children need to be able to hear in order to learn how to talk. Can ear infections be prevented? There are many ways to help prevent ear infections. Do not smoke. Ear infections happen more often to children who are around cigarette smoke. Even the fumes from tobacco smoke on your hair and clothes can affect them. Encourage hand- washing. Breastfeed your baby. Have your child immunized. Make sure your child doesn't go to sleep while sucking on a bottle. Try to limit the use of group child care. Frequently Asked Questions. Web. MD Medical Reference from Healthwise. This information is not intended to replace the advice of a doctor. Healthwise disclaims any liability for the decisions you make based on this. Healthwise, Incorporated. Healthwise, Healthwise for every health decision, and the Healthwise logo are trademarks of Healthwise, Incorporated. Ear Infections in Children | NIDCDWhat is an ear infection? An ear infection is an inflammation of the middle ear, usually caused by bacteria, that occurs when fluid builds up behind the eardrum. Anyone can get an ear infection, but children get them more often than adults. Five out of six children will have at least one ear infection by their third birthday. In fact, ear infections are the most common reason parents bring their child to a doctor. The scientific name for an ear infection is otitis media (OM). What are the symptoms of an ear infection? There are three main types of ear infections. Each has a different combination of symptoms. Acute otitis media (AOM) is the most common ear infection. Parts of the middle ear are infected and swollen and fluid is trapped behind the eardrum. This causes pain in the ear—commonly called an earache. Your child might also have a fever. Otitis media with effusion (OME) sometimes happens after an ear infection has run its course and fluid stays trapped behind the eardrum. A child with OME may have no symptoms, but a doctor will be able to see the fluid behind the eardrum with a special instrument. Chronic otitis media with effusion (COME) happens when fluid remains in the middle ear for a long time or returns over and over again, even though there is no infection. COME makes it harder for children to fight new infections and also can affect their hearing. How can I tell if my child has an ear infection? Most ear infections happen to children before they’ve learned how to talk. If your child isn’t old enough to say “My ear hurts,” here are a few things to look for: Tugging or pulling at the ear(s)Fussiness and crying. Trouble sleeping. Fever (especially in infants and younger children)Fluid draining from the ear. Clumsiness or problems with balance. Trouble hearing or responding to quiet sounds. What causes an ear infection? An ear infection usually is caused by bacteria and often begins after a child has a sore throat, cold, or other upper respiratory infection. If the upper respiratory infection is bacterial, these same bacteria may spread to the middle ear; if the upper respiratory infection is caused by a virus, such as a cold, bacteria may be drawn to the microbe- friendly environment and move into the middle ear as a secondary infection. Because of the infection, fluid builds up behind the eardrum. Parts of the ear. The ear has three major parts: the outer ear, the middle ear, and the inner ear. The outer ear, also called the pinna, includes everything we see on the outside—the curved flap of the ear leading down to the earlobe—but it also includes the ear canal, which begins at the opening to the ear and extends to the eardrum. The eardrum is a membrane that separates the outer ear from the middle ear. The middle ear—which is where ear infections occur—is located between the eardrum and the inner ear. Within the middle ear are three tiny bones called the malleus, incus, and stapes that transmit sound vibrations from the eardrum to the inner ear. The bones of the middle ear are surrounded by air. The inner ear contains the labyrinth, which help us keep our balance. The cochlea, a part of the labyrinth, is a snail- shaped organ that converts sound vibrations from the middle ear into electrical signals. The auditory nerve carries these signals from the cochlea to the brain. Other nearby parts of the ear also can be involved in ear infections. The eustachian tube is a small passageway that connects the upper part of the throat to the middle ear. Its job is to supply fresh air to the middle ear, drain fluid, and keep air pressure at a steady level between the nose and the ear. Adenoids are small pads of tissue located behind the back of the nose, above the throat, and near the eustachian tubes. Adenoids are mostly made up of immune system cells. They fight off infection by trapping bacteria that enter through the mouth. Why are children more likely than adults to get ear infections? There are several reasons why children are more likely than adults to get ear infections. Eustachian tubes are smaller and more level in children than they are in adults. This makes it difficult for fluid to drain out of the ear, even under normal conditions. If the eustachian tubes are swollen or blocked with mucus due to a cold or other respiratory illness, fluid may not be able to drain. A child’s immune system isn’t as effective as an adult’s because it’s still developing. This makes it harder for children to fight infections. As part of the immune system, the adenoids respond to bacteria passing through the nose and mouth. Sometimes bacteria get trapped in the adenoids, causing a chronic infection that can then pass on to the eustachian tubes and the middle ear. How does a doctor diagnose a middle ear infection? The first thing a doctor will do is ask you about your child’s health. Has your child had a head cold or sore throat recently? Is he having trouble sleeping? Is she pulling at her ears? If an ear infection seems likely, the simplest way for a doctor to tell is to use a lighted instrument, called an otoscope, to look at the eardrum. A red, bulging eardrum indicates an infection. A doctor also may use a pneumatic otoscope, which blows a puff of air into the ear canal, to check for fluid behind the eardrum. A normal eardrum will move back and forth more easily than an eardrum with fluid behind it. Tympanometry, which uses sound tones and air pressure, is a diagnostic test a doctor might use if the diagnosis still isn’t clear. A tympanometer is a small, soft plug that contains a tiny microphone and speaker as well as a device that varies air pressure in the ear. It measures how flexible the eardrum is at different pressures. How is an acute middle ear infection treated? Many doctors will prescribe an antibiotic, such as amoxicillin, to be taken over seven to 1. Your doctor also may recommend over- the- counter pain relievers such as acetaminophen or ibuprofen, or eardrops, to help with fever and pain. Because aspirin is considered a major preventable risk factor for Reye’s syndrome, a child who has a fever or other flu- like symptoms should not be given aspirin unless instructed to by your doctor.)If your doctor isn’t able to make a definite diagnosis of OM and your child doesn’t have severe ear pain or a fever, your doctor might ask you to wait a day or two to see if the earache goes away. The American Academy of Pediatrics issued guidelines in 2. If there’s no improvement within 4. Sometimes ear pain isn’t caused by infection, and some ear infections may get better without antibiotics. Using antibiotics cautiously and with good reason helps prevent the development of bacteria that become resistant to antibiotics. If your doctor prescribes an antibiotic, it’s important to make sure your child takes it exactly as prescribed and for the full amount of time. Even though your child may seem better in a few days, the infection still hasn’t completely cleared from the ear. Stopping the medicine too soon could allow the infection to come back. It’s also important to return for your child’s follow- up visit, so that the doctor can check if the infection is gone. How long will it take my child to get better? Your child should start feeling better within a few days after visiting the doctor. If it’s been several days and your child still seems sick, call your doctor. Your child might need a different antibiotic. Once the infection clears, fluid may still remain in the middle ear but usually disappears within three to six weeks. What happens if my child keeps getting ear infections? To keep a middle ear infection from coming back, it helps to limit some of the factors that might put your child at risk, such as not being around people who smoke and not going to bed with a bottle. In spite of these precautions, some children may continue to have middle ear infections, sometimes as many as five or six a year. Your doctor may want to wait for several months to see if things get better on their own but, if the infections keep coming back and antibiotics aren’t helping, many doctors will recommend a surgical procedure that places a small ventilation tube in the eardrum to improve air flow and prevent fluid backup in the middle ear. The most commonly used tubes stay in place for six to nine months and require follow- up visits until they fall out. If placement of the tubes still doesn’t prevent infections, a doctor may consider removing the adenoids to prevent infection from spreading to the eustachian tubes. Can ear infections be prevented? Currently, the best way to prevent ear infections is to reduce the risk factors associated with them. Here are some things you might want to do to lower your child’s risk for ear infections. Vaccinate your child against the flu. Make sure your child gets the influenza, or flu, vaccine every year. It is recommended that you vaccinate your child with the 1. PCV1. 3). The PCV1. PCV7. If your child already has begun PCV7 vaccination, consult your physician about how to transition to PCV1. The Centers for Disease Control and Prevention (CDC) recommends that children under age 2 be vaccinated, starting at 2 months of age. Studies have shown that vaccinated children get far fewer ear infections than children who aren’t vaccinated. The vaccine is strongly recommended for children in daycare. Wash hands frequently. Washing hands prevents the spread of germs and can help keep your child from catching a cold or the flu. Avoid exposing your baby to cigarette smoke. Studies have shown that babies who are around smokers have more ear infections. Never put your baby down for a nap, or for the night, with a bottle. Don’t allow sick children to spend time together. As much as possible, limit your child’s exposure to other children when your child or your child’s playmates are sick. What research is being done on middle ear infections? Ear Infection (Otitis Media). Ear Infection symptons and treatment | Health. Ear infection is very common in children, although it can occur in people of any age. The main symptoms are earache and feeling unwell. Painkillers are the main treatment. Antibiotics are not usually helpful but are prescribed in some cases. The infection usually clears within a few days. What is an ear infection? Ear infections are usually divided into those which occur in the ear canal (otitis externa) and those which occur in the small space behind the eardrum (the middle ear). You may hear an infection of the middle ear referred to as 'acute otitis media'. This leaflet deals with infections of the middle ear. How does an ear infection occur? The small space behind the eardrum in the middle ear is normally filled with air. It is connected to the back of the throat by a tiny channel called the Eustachian tube. It also contains the three tiny 'hearing bones' which pass sound through from the eardrum to the inner ear. The middle ear space should contain air but it may become filled with fluid (mucus), which typically occurs during a cold. The mucus may then become infected by germs (bacteria or viruses). This may then lead to otitis media. Children with glue ear have mucus permanently trapped behind their eardrum and they are more prone to ear infections. Sometimes an ear infection occurs 'out of the blue' for no apparent reason. What are the symptoms of an ear infection? Ear pain (earache) is common but does not always occur. It is caused by having a tense, inflamed eardrum. Dulled hearing may be present for a few days. High temperature (fever) is common. Children may feel sick or be sick (vomit) and be generally unwell. Young babies may be hot and irritable. A hot, crying baby may have an ear infection. Sometimes the eardrum bursts (perforates). This lets out the infected fluid (mucus) and often relives pain quite suddenly. The ear becomes runny, sometimes for a few days. Most perforations are small. A perforated eardrum usually heals within a few weeks after the infection clears. A note about earache. Earache is a common symptom of ear infection. However, not all earaches are caused by an ear infection. If a child has earache but is otherwise well, an ear infection is unlikely. Mild earache is often due to a build- up of mucus in the middle ear after a cold. This usually clears within a few days. Pain that you feel in the ear can be referred pain from other causes such as tooth problems or the jaw joint. What is the treatment for an ear infection? Most episodes of ear infection clear on their own without treatment and they tend to settle in 2- 3 days. The immune system can usually clear germs (bacteria or viruses) that cause ear infections. Treatments that may be advised to help with the symptoms include the following: Painkillers. If the ear infection is causing pain in your child then you can give painkillers regularly until the pain eases. For example, paracetamol (eg, Calpol®) or ibuprofen (eg, Calprofen®). These medicines will also lower a raised temperature, which can make a child feel better. If antibiotics are prescribed (see below), you should still give the painkiller as well until the pain eases. Research studies have found that a few drops of a local anaesthetic medication (lidocaine) placed into the ear may help to ease pain. Further studies are needed to clarify the use of this treatment. However, it seems logical and may become more widely used over time, especially in children with severe ear pain. Antibiotics - are prescribed in some cases only. Antibiotics are not advised in most cases. This is because the infection usually clears within 2- 3 days on its own and antibiotics make little or no difference to the speed of this. There are many good reasons not to take antibiotics. Antibiotics may cause side- effects such as runny stools (diarrhoea) or rash. They also eradicate 'friendly bacteria' from the gut, which can temporarily upset the digestive balance. Many children feel less well whilst taking antibiotics. Overuse of antibiotics encourages resistant bugs to breed, causing problems for all of us later. Antibiotics are unlikely to be helpful or justified if: Your child is 2 years old or more with a temperature of 3. C or less. Your child is not severely distressed. You child has been unwell for two days or less. Despite all this there are occasions when antibiotics are needed. Antibiotics are more likely to be prescribed if: The child is under 2 years old (as the risk of complications is greater in babies). The infection is severe. The infection is not settling within 2- 3 days. Complications develop. Your child has another medical condition (for example, diabetes) which might increase the risk of infection. When an ear infection first develops it is common for a doctor to advise a 'wait and see' approach for 2- 3 days. This means just using painkillers to ease the pain and to see if the infection clears. In most cases, the infection does clear. However, if it doesn't clear, then following a review by a doctor, an antibiotic may be advised. Sometimes, it may be difficult to see a doctor again in 2- 3 days if things do not improve - for example, over a weekend. In this situation a doctor may give you a prescription for an antibiotic with the advice to use it to obtain the antibiotic only if the condition does not improve within 2- 3 days. What are the possible complications from an ear infection? It is common for some fluid (mucus) to remain behind the eardrum after the infection clears. This may cause dulled hearing for a while. This usually clears within a week or so and hearing then returns to normal. Sometimes the mucus does not clear properly and 'glue ear' may develop. Hearing may then remain dulled. Repeated ear infections (for example, due to having several colds in a row) can lead to glue ear. See a doctor if dulled hearing persists after an ear infection has gone, or if you suspect your child is having difficulty hearing. If the eardrum bursts (perforates) then it usually heals over within a few weeks once the infection clears. In some cases the perforation remains long- term and may need treatment to fix it. If a child is normally healthy then the risk of other serious complications developing from an ear infection is very small. Rarely, a serious infection of the bone behind the ear develops from an ear infection. This is called mastoiditis. Very rarely, the infection spreads deeper into the inner ear, brain or other nearby tissues. This can cause various symptoms that can affect the brain and nearby nerves, including abscess and meningitis. You should always consult a doctor if a child with earache: Becomes more ill. Has an illness which seems severe to you. Does not improve over 2- 3 days. Has a temperature above 3. C. A fever like this is not generally considered a danger to your child. Children develop high temperatures in many common illnesses, including ear infections, urinary tract infections, roseola (a common childhood virus) and flu. However, when the temperature is above 3. C your child is more likely to have an illness or infection that needs your doctor's help. If your child is under 3 months old then you should see a doctor if their temperature is above 3. C). Develops any symptoms that you are not sure about. Will it happen again and can it be prevented? Most children have at least two bouts of ear infection before they are 5 years old. These are caused by common viral infections which circulate in the general population and against which your child is not immune. There is generally nothing you can do to prevent the infection from occurring. However, there is some evidence to suggest that an ear infection is less likely to develop: In breast- fed children. In children who live in a smoke- free home. Passive smoking of babies and children can increase the risk of developing ear infections.)In babies and young children who do not use dummies. However, research studies have shown that the use of a dummy in young babies when getting off to sleep can reduce the risk of cot death. So, consider using a dummy in babies up to 6- 1. If you breast- feed, do not start to use a dummy until you are well established with breast- feeding. This is normally when the baby is about one month old.) But note: Do not force a dummy on a baby who does not want one. If the dummy falls out when a baby is asleep, just leave it out. Never coat a dummy with anything such as sugar. Clean and replace dummies regularly. It is best to use a dummy only to help a baby get to sleep. Consider stopping dummy use at around 6- 1. Occasionally, some children have recurring bouts of ear infections close together. If this occurs, a specialist may advise a long course of antibiotics to prevent further bouts from occurring. If infections are very frequent, a specialist may advise the insertion of a grommet into the eardrum. This is the same treatment that is used to treat some cases of glue ear. A grommet is like a tiny drainage pipe that helps to let fluid escape from the middle ear, and that lets air in. Some research suggests that this may reduce the number of ear infections that occur. See separate leaflet called Operations for Glue Ear for more details.
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
